For many individuals, anatomic total shoulder replacement surgery provides meaningful relief from arthritis-related pain and stiffness. However, like any major procedure, it carries potential risks. Understanding the possible problems after shoulder replacement surgery can help you make informed decisions and recognize concerns early. In this post, we’ll review the complications that may follow total shoulder replacement, with a focused look at glenoid loosening, why it occurs, how it presents, and the technology designed to reduce its likelihood.
Key Takeaways
- Glenoid loosening is considered one of the most common long-term reasons an anatomic total shoulder replacement may eventually require revision.
- Newer implant designs aim to significantly reduce the mechanical stresses that contribute to loosening.
- Partnering with a fellowship-trained shoulder surgeon who utilizes advanced preoperative planning tools may improve surgical precision and outcomes.
The Basics of Anatomic Total Shoulder Replacement
Your shoulder functions as a ball-and-socket joint. The ball portion, formed by the top of your upper arm bone, called the humeral head, fits into a shallow dish on the shoulder blade known as the glenoid. Cartilage coats both sides, supporting smooth and pain-free movement. When arthritis erodes that cartilage, pain takes over and range of motion often declines.
In this procedure, a surgeon takes out the worn cartilage and bone surfaces and replaces them with prosthetic components. The aim is to recreate the joint’s natural anatomy so that it can move comfortably again. Most patients report improvement in both pain and function after recovery, though individual results vary.
Why Complications May Develop After Surgery
No joint replacement is immune to complications. Factors like bone quality, the patient’s activity level, implant positioning, and even the design of the prosthesis itself all play a role. Some complications appear within weeks of the procedure. Others develop gradually over years. Among all the potential problems after shoulder replacement surgery, glenoid loosening consistently stands out as a leading long-term mechanical concern.
Glenoid Loosening
Glenoid loosening refers to the gradual separation of the socket implant from the bone beneath it. It is widely reported as one of the most common reasons patients may require revision surgery after an anatomic total shoulder replacement.
What Drives the Loosening Process
Older glenoid implant designs are positioned directly on the surface of the bone. Each time you raise your arm, reach overhead, or rotate your shoulder, forces are transmitted through the plastic component. Over time, this can lead to a subtle back-and-forth tilting motion, often referred to as the “rocking horse” effect. This repetitive tilting concentrates stress along the edges of the component, gradually weakening the bond between implant and bone.

The loosening process does not usually happen all at once. In its earliest phase, microscopic movement occurs at the bone-implant boundary. As those tiny gaps expand, the body may begin to resorb bone in the surrounding area, a process referred to as osteolysis. Cracks can form in the cement layer, and you might start to notice subtle changes like mild discomfort or a feeling that your shoulder is not as dependable as it once was.
If the loosening continues, symptoms generally become more noticeable. Pain may resurface or intensify during activity. You might experience decreased range of motion, grinding sensations, or clicking. In advanced cases, imaging may reveal that the component has shifted from its original position, and a second operation may be needed to address the problem.
Who Faces a Higher Risk?
A number of patient-specific and surgical factors may shape the likelihood of loosening over time. Individuals with weaker or less dense bone at the time of their procedure may struggle to achieve solid initial implant fixation. Alignment is another key variable, as even slight deviations in how the component is angled can change where stress concentrates during everyday shoulder use. How actively a patient uses the joint also matters. Repeated heavy loading may speed up wear. Some people maintain well-fixed glenoid components for more than a decade, while others notice changes sooner.
How Modern Systems Aim to Combat Glenoid Loosening
Because glenoid loosening has long been recognized as a major obstacle in shoulder arthroplasty, considerable engineering effort has gone into developing better implant designs. The InSet® Shoulder System from Shoulder Innovations represents one of the more notable advances.
The core difference lies in how the glenoid component interfaces with your bone. Instead of being mounted on the outer bone surface, the InSet® glenoid is seated within a prepared pocket of dense, sclerotic bone in the shoulder blade. The concept draws inspiration from an everyday object: a manhole cover. Heavy vehicles drive across manhole covers every day, yet the covers stay securely in place because they sit flush within a rim of surrounding material.

That design principle translates into measurable mechanical advantages. In Finite Element Analysis, a type of computer-based mechanical simulation, this approach showed as much as an 87% decrease in the rocking horse stresses tied to conventional loosening. By surrounding the component with a protective ring of strong bone, the InSet® design helps distribute forces more evenly and resists the tilting motion that typically undermines traditional implants. This is one of the reasons I use this system in my own practice.
Precision Planning with Advanced Software
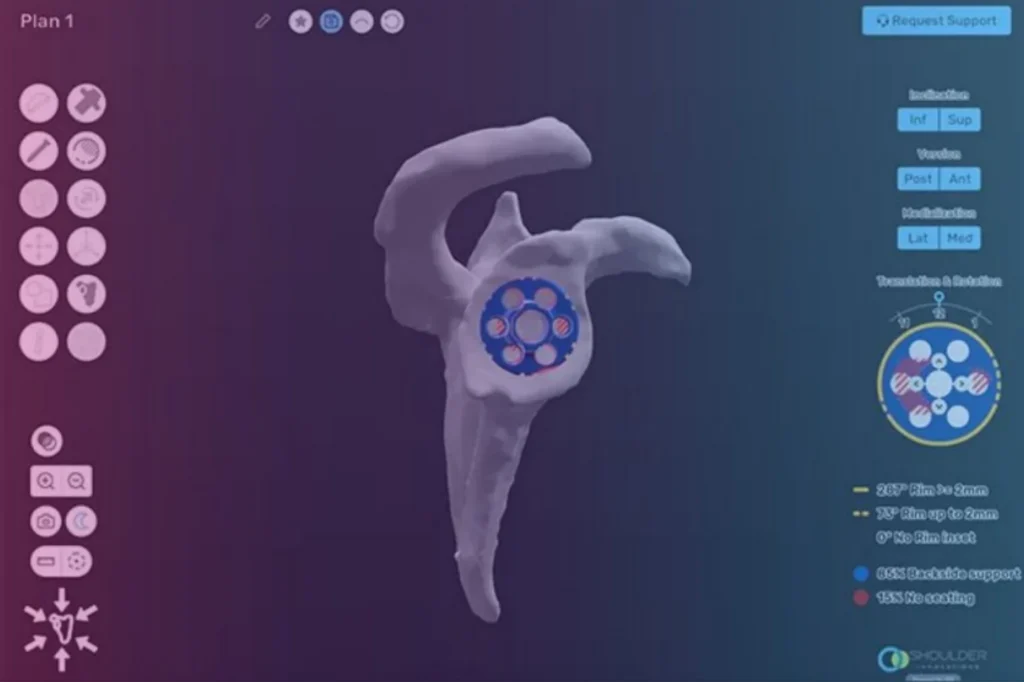
Implant design is only one piece of the puzzle. Where a surgeon places each component, and at what angle, matters enormously for long-term stability. I use ProVoyance®, an advanced 3D surgical planning platform, to map out the optimal size, position, and orientation of each implant before the procedure begins. This patient-specific approach uses detailed imaging of each individual’s anatomy and may help reduce the likelihood of implant malpositioning, which is one factor that can contribute to loosening and other complications.
Other Complications That May Follow a Shoulder Replacement
While glenoid loosening tends to dominate the conversation around problems after total shoulder replacement surgery, it is not the only complication worth understanding. Being informed about other potential risks can help you and your care team identify issues early.
Infection
An infection can remain superficial, affecting only the incision area, or it can reach deeper into the joint. Deep infections may require additional procedures to clean the affected tissue, and in some situations, the implant may need to be temporarily removed. Keep an eye out for worsening pain, redness, swelling, warmth near the wound, discharge, or fever. Contacting your surgeon quickly if you notice any of these signs gives your team the best opportunity to intervene early.
The most common organism that causes infection after shoulder replacement surgery is called Cutibacterium acnes or C. acnes (pronounced “see ack nees”). C. acnes infection may not result in the usual symptoms of infection such as fever, redness, drainage or abnormal blood work. The only abnormality may be low grade pain, loss of motion, or changes around the implant by x-rays. C. acnes bacteria live in the layer of human skin called the dermis, specifically in the hair follicles and sweat glands. It is therefore difficult to eradicate from the surgical field. The “burden” of this bacteria can be reduced prior to surgery through special skin washing with benzoyl peroxide solutions, which are commercially available as acne face washes. Infection with C.acnes after shoulder replacement surgery is more common in men, especially men who are on testosterone therapy, whether self-prescribed or physician-directed. It is important to report any testosterone therapy to your shoulder specialist, as this should be held for some time prior to and after shoulder replacement surgery in order to minimize the risk of infection with C. acnes.
Instability and Dislocation
After replacement, the prosthetic ball needs to remain properly seated within the socket. If it shifts, the joint becomes unstable. In more serious situations, a full dislocation can occur. Careful component sizing, accurate positioning, and appropriate soft tissue balancing during surgery all help mitigate this risk. Your rotator cuff and the surrounding muscular structures also play a role in keeping the joint stable. Symptoms can include a feeling of the joint wanting to give out or an audible clunk when you move your arm.
Nerve Injury
Several nerves responsible for shoulder movement and sensation run in close proximity to the surgical field. The axillary nerve is especially worth noting because it powers the deltoid muscle and sits near the operative area. Most nerve injuries following shoulder replacement are temporary and tend to improve over weeks to months. Symptoms may include numbness, tingling, or weakness in the affected area.
Rotator Cuff Issues
Your rotator cuff, the collection of tendons responsible for stabilizing and powering your shoulder, continues to play a key role after replacement. A tear in one of these tendons can compromise joint function and may contribute to instability. Some patients already have rotator cuff damage heading into surgery, and that damage can sometimes progress over time.
Prolonged Stiffness
A degree of stiffness in the first several weeks after surgery is expected and normal. However, stiffness that lingers well beyond the early recovery period and interferes with routine tasks may point to an underlying issue. Buildup of scar tissue, insufficient rehabilitation participation, or suboptimal component placement can all contribute. Staying consistent with your physical therapy program is one of the most effective strategies for preventing this issue.
Steps You Can Take to Protect Your Outcome
While no surgeon can guarantee a complication-free experience, there are proactive measures that may tip the scales in your favor. Here are the areas I encourage patients to focus on.
Select a Shoulder Specialist with Focused Experience
Shoulder replacement is a technically intricate procedure. Surgeon experience and case volume are factors often associated with improved surgical consistency and outcomes. When you meet with a potential surgeon, do not hesitate to ask about their training, how many shoulder replacements they perform each year, and which implant systems they use.
Optimize Your Health Before the Procedure
Going into surgery in the best health possible can make a real difference. Work with your doctor to manage any chronic conditions such as diabetes or hypertension. If you smoke, consider quitting at least several weeks before the procedure, as smoking may impair healing and increase the risk of complications.
Follow Through with Rehabilitation
Physical therapy tends to play a central role in recovery. In the early weeks, sessions typically focus on gentle passive movements to protect healing tissues. As recovery progresses, your therapist will introduce active exercises aimed at rebuilding strength and restoring range of motion. Showing up consistently, both to scheduled sessions and to your home exercise program, can make a meaningful difference in your final outcome.
Respect Long-Term Activity Guidelines
Modern shoulder implants are built to be durable, but they do have limits. Collision sports, aggressive overhead lifting, and high-force repetitive motions can place excessive stress on the prosthetic components. Lower-impact pursuits such as swimming, golf, and walking tend to be well-tolerated. Have an open conversation with your surgeon about your specific activity goals so that you can set realistic expectations.
Stay in Close Contact with Your Surgical Team
Open communication with your surgeon is one of the most underrated tools in your recovery toolkit. Do not wait for a scheduled appointment if something feels off. Problems after shoulder replacement surgery are generally easier to address when caught early.
Summary
Total shoulder replacement continues to provide meaningful relief for many patients struggling with arthritis and shoulder damage. That said, problems after shoulder replacement surgery remain a possibility, and glenoid loosening stands as the most commonly reported long-term mechanical complication of anatomic shoulder replacement.
Advances in implant engineering represent an encouraging step forward in reducing loosening risk. Combined with precise surgical planning and the expertise of a fellowship-trained shoulder surgeon, these advances provide patients with multiple strategies aimed at supporting long-term stability and function. Your own commitment to pre-surgical preparation, consistent rehabilitation, and ongoing communication with your surgical team also plays a meaningful role in long-term success.
Frequently Asked Questions
What is glenoid loosening, and why is it a concern?
Glenoid loosening happens when the polyethylene socket implant progressively separates from the bone of the shoulder blade. This complication is widely recognized as the leading mechanical cause of revision in anatomic shoulder replacements. As the implant detaches over time, patients may notice returning pain and declining function.
Which activities should I avoid after a total shoulder replacement?
Most shoulder surgeons advise against collision sports, aggressive overhead lifting, and high-force activities that could overload the prosthetic components. Situations where you might fall should also be navigated with extra care. Lower-impact options like swimming, golf, and walking tend to be well-suited for patients with a shoulder replacement. Your surgeon can offer guidance specific to your situation.
Should I be concerned about pain after shoulder replacement?
Some discomfort during the initial healing period is expected and normal. This should gradually diminish over the weeks and months following surgery. However, pain that intensifies, comes back after a period of improvement, or accompanies other concerning signs should be discussed with your surgeon. When in doubt, it is always better to reach out.

